The post Optimal Nutrients for Pregnancy and Baby Health appeared first on .
]]>
INTRODUCTION
A healthy diet during pregnancy is essential for the well-being of both the mother and the developing baby. The right nutrients support the baby’s growth, development, and overall health while also helping the mother maintain her energy, manage changes, and prepare for childbirth. Pregnancy places additional demands on the body, making it crucial to focus on specific nutrients that are required in higher amounts during this time. During pregnancy, a woman’s body goes through various physiological transformations that help the fetus grow and also prepare both for labor and delivery. (1,2)
Certain nutrients play a particularly important role in a healthy pregnancy. For example, folic acid is vital in the early stages to reduce the risk of neural tube defects, while iron helps prevent anemia by supporting the increased blood volume. Calcium and vitamin D work together to support the development of the baby’s bones and teeth. Protein is essential for tissue growth, and omega-3 fatty acids support brain and eye development.
A pregnancy diet should also include an appropriate balance of carbohydrates, healthy fats, fiber, and vitamins and minerals to meet the growing nutritional needs. Eating a variety of nutrient-rich foods such as whole grains, lean proteins, fruits, vegetables, and dairy products ensures that both the mother and the baby receive the necessary nutrients.
Pregnant women should aim to maintain a balanced and nutrient-rich diet, minimizing the intake of unhealthy foods and prioritizing whole, unprocessed options. Working with a healthcare provider or nutritionist can help customize the diet to meet the unique needs of the pregnancy, promoting a safe and healthy journey for both the mother and the baby.
Essential nutrients required during pregnancy:
- Folic acid or Folate: Prevent brain and spinal cord birth problems
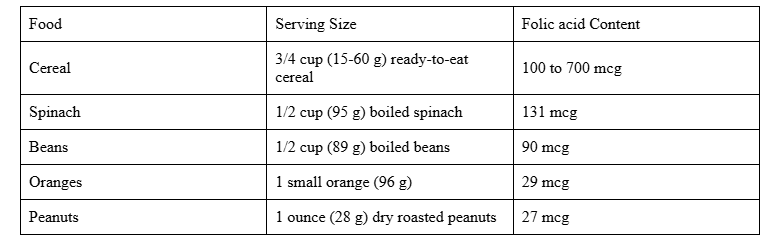
Folate, a type of B vitamin, plays a crucial role in preventing severe issues in the developing brain and spinal cord, such as neural tube defects. Its synthetic version, found in fortified foods and supplements, is called folic acid. Taking folic acid has been proven to reduce the chances of premature birth and low birth weight in babies.
Recommended Intake: Before conception, you need 400 micrograms (mcg) of folate or folic acid daily to support healthy development. During pregnancy, this requirement increases to 600–1,000 mcg per day to ensure proper growth and reduce the risk of neural tube defects in your baby.
- Calcium: Strengthen bones
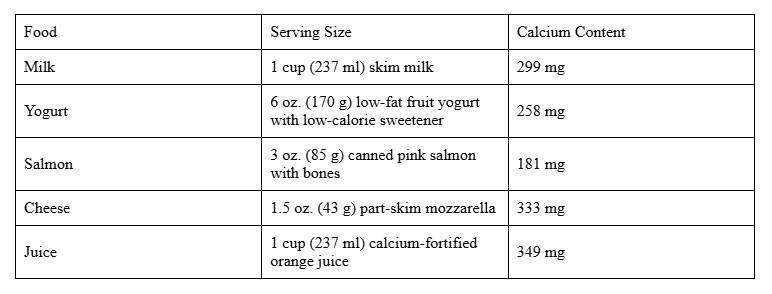
Both you and your baby require calcium to build and maintain strong bones and teeth. In addition to this, calcium is essential for the proper functioning of the circulatory, muscular, and nervous systems. It also plays a vital role in blood clotting, hormone release, and ensuring your baby’s overall healthy growth and development during pregnancy.
Recommended Intake: Pregnant women require 1,000 milligrams (mg) of calcium daily to support their baby’s bone and teeth development, while pregnant teenagers need a slightly higher intake of 1,300 mg per day to meet their growing bodies’ additional needs.
- Vitamin D: Promote bone strength
Vitamin D works hand in hand with calcium to support the formation of your baby’s strong bones and healthy teeth. It also plays a crucial role in helping the body absorb calcium effectively, promoting proper skeletal development and reducing the risk of bone-related issues for both you and your baby.
Recommended Intake: It is recommended to consume 600 international units (IU) of vitamin D daily during pregnancy to support your baby’s bone development and overall health, as well as to aid calcium absorption in your body.

- Protein: Promote growth
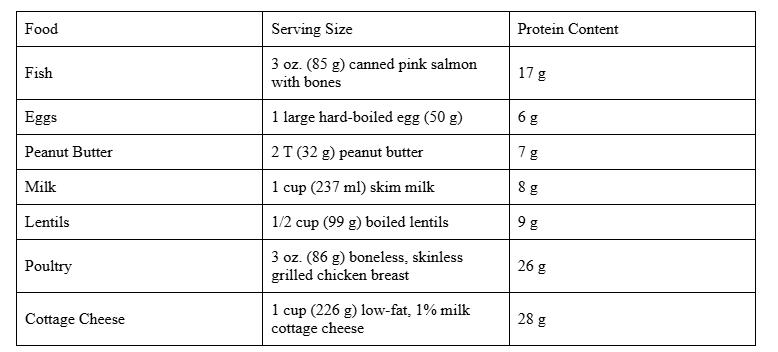
Protein is essential for your baby’s growth and development throughout pregnancy, as it supports the formation of new cells, tissues, and organs. It also plays a key role in building the placenta, ensuring proper nutrient transfer to your baby, and maintaining your own health during this critical time.
Recommended Intake: During pregnancy, you should aim to consume 71 grams (g) of protein daily. This helps support your baby’s growth, the development of tissues and organs, and the increased demands of your own body during this critical time.
- Iron: Prevent iron deficiency anemia
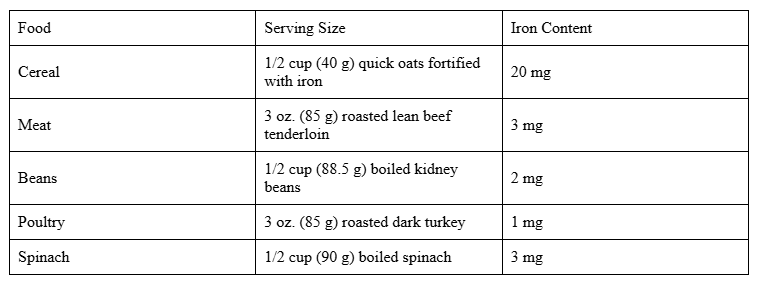
Iron is essential for the production of hemoglobin, a protein in red blood cells responsible for carrying oxygen to the body’s tissues. During pregnancy, your body requires twice as much iron as usual to produce extra blood needed to supply oxygen to your growing baby.
If your iron levels are too low or your stores are insufficient, you may develop iron deficiency anemia. This can lead to symptoms such as fatigue, weakness, and headaches. Severe cases during pregnancy can increase the risk of complications, including premature birth, low birth weight, and postpartum depression.
Recommended Intake: During pregnancy, it is recommended to get 27 milligrams (mg) of iron daily. This helps support the increased blood volume needed to carry oxygen to both you and your baby, reducing the risk of iron deficiency anemia.
- Omega-3 fatty acids: Supports brain development
Omega-3 fatty acids are a type of healthy fat found naturally in several fish, such as salmon, mackerel, and sardines, and play a vital role in supporting brain development before and after birth. These essential fats are also important for reducing inflammation and promoting overall health. Flaxseed, whether ground or in oil form, is an excellent plant-based source of omega-3s. In addition, omega-3s can be found in a variety of other foods, including broccoli, cantaloupe, kidney beans, spinach, cauliflower, and walnuts, making it easier to include these healthy fats in your diet.
Recommended Intake: The recommended intake of omega-3 fatty acids during pregnancy is about 200-300 milligrams (mg) per day of DHA (a type of omega-3) to support the development of your baby’s brain and eyes.
For non-pregnant individuals, a general recommendation is 250-500 mg of combined EPA and DHA per day for overall health.
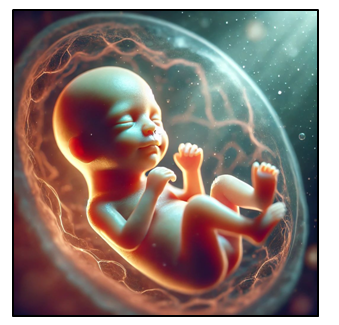
Weight Gain: What’s Normal?
If you’re worried about gaining weight during pregnancy, try not to stress. It’s completely natural to gain some weight, as it supports the baby’s nourishment. A portion of this weight is also stored to help with breastfeeding once the baby is born.
On average, women gain about 25 to 35 pounds during pregnancy. However, the amount of weight gained can vary. Women who are underweight before pregnancy may gain more, while those with higher pre-pregnancy weight may gain less.
Ideal Weight Gain during Pregnancy with One Baby:
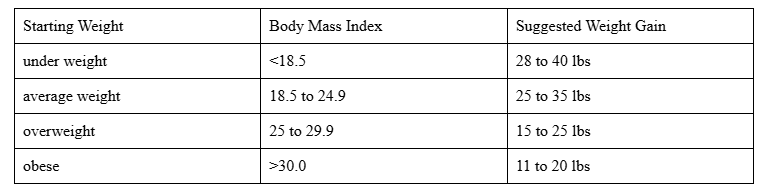
What foods should be restricted during pregnancy?
- Alcohol: There is no known safe amount of alcohol to consume during pregnancy.
- Fish with high mercury levels: Limit white (albacore) tuna to 6 ounces per week, and avoid eating tilefish, shark, swordfish, marlin.
- Foods that could carry harmful germs: These include:
- Refrigerated smoked seafood, such as whitefish, and mackerel
- Undercooked meat, poultry, eggs, and seafood
- Refrigerated meat spreads
- Pre-made salads like chicken, egg, or tuna salad
- Unpasteurized or raw milk
- Unpasteurized juices or cider
- Soft cheeses made from unpasteurized milk
- Raw sprouts of any kind (such as alfalfa, clover, radish, and mung beans)
- Raw cookie dough
- Unwashed fruits and vegetables
- Excessive caffeine: Drinking too much caffeine may harm your baby. It’s recommended to limit caffeine under 200 mg per day during pregnancy.
GESTATIONAL DIABETES
Gestational diabetes is a condition characterized by high blood sugar that develops or is first detected during pregnancy. Women with gestational diabetes are more likely to give birth to larger babies, which can lead to complications during delivery.
The goals of Medical Nutrition Therapy (MNT) in Gestational Diabetes include:
- The meal plan should ensure sufficient calories and nutrients to meet both maternal and fetal needs in pregnancy.
- Caloric requirements vary based on factors such as age, activity level, pre-pregnancy weight, and the stage of pregnancy.
- During the second and third trimesters, an increase of 350 kcal above the baseline requirement, or approximately 30-40 kcal per kilogram of ideal body weight, is recommended.
Diet management plan for pregnant woman experiencing vomiting:
Vomiting leads to the loss of fluids and electrolytes in the body, so the primary focus should be on keeping the pregnant woman properly hydrated.
To achieve this:
- Drink fluids in small sips throughout the day, such as electrolyte drinks, lemonade, or diluted fruit juices.
- Consume snacks with high water content like watermelon, canned fruit, fruit juice bars, or flavored ice cubes.
- Easy-to-Digest Foods:
- Eat low-fat, bland foods like crackers, rice, toast, and boiled potatoes.
- Avoid spicy, greasy, or strong-smelling foods.
- Small, Frequent Meals:
- Have small meals every 2-3 hours to prevent nausea, like applesauce, plain yogurt, or oatmeal.
- Use Ginger and Vitamin B6:
- Try ginger in tea, candies, or ginger ale to help reduce nausea.
- Consider Vitamin B6 (with medical advice) for relief.
- Avoid Strong Odors: Steer clear of foods with strong smells to prevent triggering nausea.
During pregnancy, constipation is a common issue. To manage constipation during pregnancy, the following dietary changes can be helpful:
- Increase Fruit and Vegetable Intake: Eat plenty of fiber-rich fruits and vegetables to promote regular bowel movements.
- Stay Hydrated: Drink plenty of fluids throughout the day to help soften stool and prevent dehydration.
- Avoid Mineral Oils and Natural Remedies: Refrain from using mineral oils or other natural remedies, as they can have unwanted effects during pregnancy.
- Avoid Laxatives: Do not use laxatives, unless advised by a healthcare provider, as they may not be safe during pregnancy. (3)
REFERENCES
- Heidemann B.H., McClure J.H. Changes in maternal physiology during pregnancy. BJA CEPD Rev. 2003;3:65–68. doi: 10.1093/bjacepd/mkg065.
- Soma-Pillay P., Nelson-Piercy C., Tolppanen H., Mebazaa A. Physiological changes in pregnancy. Cardiovasc. J. Afr. 2016;27:89–94. doi: 10.5830/CVJA-2016-021.
- Seshiah et al. Gestational Diabetes Mellitus – Indian Guidelines. JAPI, Vol. 54 August, 2006.
The post Optimal Nutrients for Pregnancy and Baby Health appeared first on .
]]>The post DIABETES MELLITUS (DM) appeared first on .
]]>The word Diabetes mellitus is derived from both the Greek and Latin word. Diabetes is taken from the Greek word “diabainein”, which means “to pass through” or “siphon” and “Mellitus” is the Latin word which refers to honey- like sweetness. The word “diabetes” was originally coined by Apollonius of Memphis around 250-300 BC. Globally and nationally, diabetes is considered one of the most widespread and chronic conditions, In the United States, it is still the seventh leading reason of death.
Diabetes mellitus is a metabolic disorder characterized by increased blood sugar (glucose) levels due to the lack of body’s ability to produce adequate insulin. There are various types of DM including gestational diabetes, type 1 diabetes, type 2 diabetes, neonatal diabetes, etc. But the main subtypes are type 1 diabetes mellitus (T1DM) and type2 diabetes mellitus (T2DM).(1) T1DM is commonly found in children or teenager, whereas T2DM is predominantly seen in older and middle aged individuals, who may experience sustained elevated blood sugar levels due to unhealthy lifestyle and eating habits.
TYPES OF DIABETES MELLITUS
- TYPE 1 DIABETES
Formerly known as juvenile diabetes, It occurs when the immune system attacks and kills the Beta cells present in the pancreas-the only cells in the body that is responsible for producing insulin.(2,3) In this chronic condition, the pancreas produces a small amount or no insulin, depending on how many Beta cells in the pancreas are not functioning. There is no way to cure and prevent type 1 diabetes. These patients are required to take insulin injections for their entire lives. They should also monitor their blood glucose level by consistently checking and following a specific diet plan.
Some medicines or drugs that are responsible for reducing insulin secretion and damaging Beta cells include:
- Antiviral drug: Didanosine
- Anti-protozoal drug: Pentamidine
- Antibiotic drug: Gatifloxicin
- Leukemia drug: L – asparaginase
- TYPE 2 DIABETES
Formerly known as adult-onset diabetes, it occurs when cells in the body are unable to respond to insulin, making it challenging for glucose to enter the cells. The primary cause of type 2 diabetes are excessive weight and lack of physical activity. There is no cure for type 2 diabetes but it can be prevented by maintaining a healthy weight, regular exercise and by following a nutritious dietary plan. If blood sugar is not be controlled by diet and exercise then diabetes medications or insulin therapy could be recommended.
Symptoms and complications of Diabetes mellitus
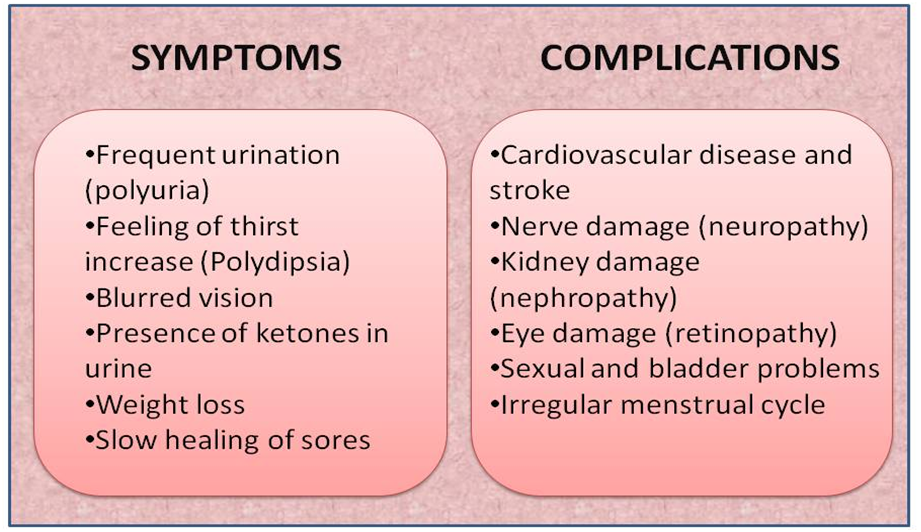
GLUCOMETER
In 1971, a German engineer Anton Hubert Clemens was the first person who invented the glucose meter, also known as glucometer, it is a machine which is used in the determination of glucose concentration in blood. The normal range of blood glucose in fasting condition is 80-130 mg/dL and 2 hours after meal is less than 180 mg/dL.

BLOOD GLUCOSE LEVEL CLASSIFICATION: Normal, Prediabetes and Diabetes
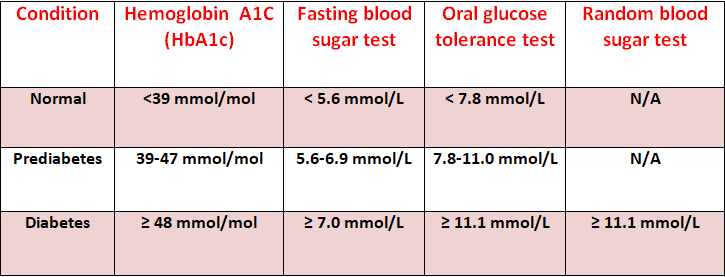
CLASSIFICATION OF ORAL ANTIDIABETIC DRUGS
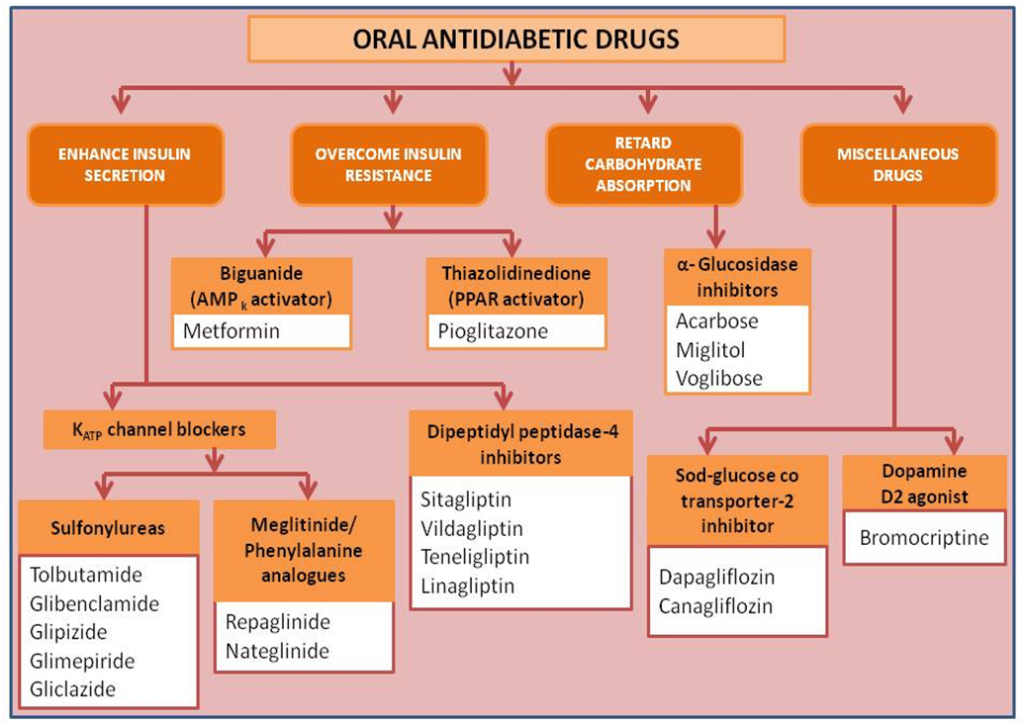
CONCLUSION
In conclusion, diabetes mellitus is a chronic disorder which affects the body’s regulation process of glucose, resulting in high blood sugar. It is an increasing health issue worldwide, with different types like Type 1, Type 2, and gestational diabetes. While there is no cure of diabetes mellitus, it can be managed through lifestyle changes, medication, and monitoring glucose levels. Early diagnosis, a balanced diet, and regular exercise are essential for improving the quality of life for individuals with diabetes.
REFRENCE
1. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2014;37 Suppl 1:S81–S90. [PubMed] [Google Scholar]
2. Daneman D. Type 1 diabetes. Lancet. 2006;367:847–858. [PubMed] [Google Scholar]
3. Devendra D, Liu E, Eisenbarth GS. Type 1 diabetes: recent developments. BMJ. 2004;328:750–754. [PMC free article] [PubMed] [Google Scholar]
The post DIABETES MELLITUS (DM) appeared first on .
]]>The post Revolutionizing Healthcare: The Rise of Personalized Medicine appeared first on .
]]>
Table of Contents:
- Introduction to Personalized Medicine
- The Science Behind Personalized Medicine
- Genomics and Genetics
- Proteomics and Metabolomics
- Biomarkers in Personalized Medicine
- How Personalized Medicine Differs from Traditional Medicine
- Key Components and Technologies Driving Personalized Medicine
- Artificial Intelligence and Machine Learning
- Big Data Analytics in Healthcare
- Next-Generation Sequencing (NGS)
- CRISPR and Gene Editing
- Personalized Medicine in Cancer Treatment
- Precision Oncology
- Targeted Therapies
- Immunotherapies
- Personalized Medicine in Other Disease Areas
- Cardiovascular Diseases
- Neurological Disorders
- Rare Genetic Diseases
- Pharmacogenomics: Tailoring Drug Therapy
- The Role of Genetics in Drug Response
- Case Studies in Pharmacogenomics
- Benefits of Personalized Medicine for Patients and Healthcare Providers
- Improved Patient Outcomes
- Cost-Effectiveness
- Preventive Care and Early Diagnosis
- The Ethical, Legal, and Social Implications of Personalized Medicine
- Data Privacy and Security
- Access and Equity
- The Role of Informed Consent
- Personalized Medicine and Patient Empowerment
- How Personalized Medicine Involves Patients in Their Own Care
- The Role of Patient Advocacy
- Future Prospects: What’s Next for Personalized Medicine?
- Emerging Technologies and Innovations
- Precision Health: Moving Beyond Treatment to Prevention
- Challenges and Barriers in Implementing Personalized Medicine
- Healthcare System Barriers
- Cost and Reimbursement Issues
- Integrating Personalized Medicine into Everyday Clinical Practice
- Conclusion: The Transformative Power of Personalized Medicine
Introduction to Personalized Medicine
Personalized medicine represents a groundbreaking approach to healthcare, where medical decisions, treatments, and practices are tailored to the individual patient based on their genetic makeup, lifestyle, and environment. This shift from a “one-size-fits-all” model to one that considers the unique biological factors of each patient is reshaping how we approach disease prevention, diagnosis, and treatment.
Personalized medicine aims to predict which medical treatments will be most effective for each patient, minimizing adverse reactions and maximizing positive outcomes. Advances in fields such as genomics, proteomics, and bioinformatics are enabling this transformation, offering new opportunities for tailored therapies that target specific diseases at a molecular level.
The Science Behind Personalized Medicine
Genomics and Genetics The cornerstone of personalized medicine lies in our understanding of genetics. Human beings share approximately 99.9% of their DNA, but it is the remaining 0.1% that accounts for variations in disease susceptibility, drug response, and other health-related factors. By studying a patient’s genome, doctors can identify genetic variants that may contribute to the risk of developing certain conditions or influence how an individual might respond to a particular drug.
Proteomics and Metabolomics Beyond genomics, the study of proteins (proteomics) and metabolites (metabolomics) also plays a critical role in personalized medicine. Proteins are the functional molecules in the body that drive biological processes, and understanding their structure and function is crucial for identifying disease biomarkers. Metabolomics focuses on the unique chemical fingerprints left behind by cellular processes, providing insights into the dynamic biochemical changes within the body.
Biomarkers in Personalized Medicine Biomarkers are biological molecules that indicate the presence of a disease or the response of the body to treatment. They are essential tools in personalized medicine, offering physicians valuable insights into disease progression and patient response to therapies. Biomarkers can be genetic, proteomic, or metabolomic in nature, and their discovery has been critical in the development of personalized treatments.
How Personalized Medicine Differs from Traditional Medicine
Traditional medicine often employs a generalized treatment approach, where patients with similar symptoms receive similar treatments. However, not all patients respond to the same treatment in the same way, leading to varying outcomes. Personalized medicine, on the other hand, uses detailed patient data to tailor medical care to each individual, improving the effectiveness of treatments and minimizing side effects.
In traditional medicine, therapies are developed and tested based on population averages, which may not always apply to individual patients. Personalized medicine focuses on the individual, using predictive tools to assess the likelihood of success for a particular treatment, and sometimes even developing customized therapies based on the patient’s unique profile.
Key Components and Technologies Driving Personalized Medicine
Artificial Intelligence and Machine Learning AI and machine learning are revolutionizing the field of personalized medicine by enabling the analysis of vast datasets, including genomic information, electronic health records, and real-time patient data. These technologies help identify patterns and correlations that might not be visible through traditional methods, accelerating the discovery of new treatment options.
Big Data Analytics in Healthcare The volume of healthcare data generated today is staggering, and big data analytics plays a crucial role in harnessing this information for personalized medicine. By analyzing large-scale datasets from diverse patient populations, researchers can identify trends, predict outcomes, and develop more effective treatment strategies tailored to individual patients.
Next-Generation Sequencing (NGS) Next-generation sequencing (NGS) has dramatically reduced the cost and time required for genomic sequencing, making it a critical tool in personalized medicine. NGS allows for the rapid analysis of a patient’s entire genome, enabling the identification of genetic mutations or variants that may impact disease risk or treatment response.
CRISPR and Gene Editing The CRISPR-Cas9 gene-editing technology has opened up new possibilities in personalized medicine by enabling the precise modification of genetic material. With CRISPR, scientists can target and edit specific genes that contribute to disease, potentially offering cures for genetic disorders. While the use of CRISPR in clinical settings is still in its early stages, it holds tremendous promise for personalized therapies.
Personalized Medicine in Cancer Treatment
Precision Oncology Cancer treatment has been one of the biggest beneficiaries of personalized medicine. Precision oncology tailors cancer treatments based on the genetic makeup of an individual’s tumor, allowing for the selection of therapies that are more likely to be effective. Advances in cancer genomics have led to the development of targeted therapies that attack cancer cells while sparing healthy ones.
Targeted Therapies Targeted cancer therapies focus on specific molecules within cancer cells that drive tumor growth. By targeting these molecules, these therapies can more effectively kill cancer cells while reducing damage to surrounding healthy tissue. Personalized medicine has made it possible to match patients with the targeted therapies that are most likely to work based on the genetic characteristics of their tumor.
Immunotherapies Immunotherapy has become a promising avenue in cancer treatment, harnessing the patient’s immune system to fight the disease. Personalized immunotherapies, such as CAR-T cell therapy, are designed to recognize and attack cancer cells with precision, offering new hope for patients with certain types of cancer.
Personalized Medicine in Other Disease Areas
Cardiovascular Diseases Personalized medicine is making strides in cardiovascular care by identifying genetic factors that influence heart disease risk and treatment response. For example, pharmacogenomic testing can help determine how patients with cardiovascular conditions will respond to blood thinners or cholesterol-lowering medications, allowing for more precise dosing and better outcomes.
Neurological Disorders Neurological conditions, such as Alzheimer’s disease and Parkinson’s disease, have complex genetic and environmental causes. Personalized medicine is helping researchers identify biomarkers that can predict the risk of developing these conditions, enabling earlier intervention and more effective treatments.
Rare Genetic Diseases For patients with rare genetic diseases, personalized medicine offers new hope through therapies that target the underlying genetic cause of their condition. Advances in gene therapy and gene editing have made it possible to develop treatments that address the root cause of rare diseases, improving quality of life for patients.
Pharmacogenomics: Tailoring Drug Therapy
The Role of Genetics in Drug Response Pharmacogenomics studies how an individual’s genetic makeup influences their response to drugs. Variations in certain genes can affect how a person metabolizes medications, leading to differences in drug efficacy and the likelihood of side effects. By understanding a patient’s genetic profile, doctors can select the right drug and dosage for optimal results.
Case Studies in Pharmacogenomics Several case studies have demonstrated the potential of pharmacogenomics to improve patient outcomes. For example, patients with certain genetic mutations may metabolize common painkillers, like codeine, too quickly or too slowly, leading to dangerous side effects or inadequate pain relief. Pharmacogenomic testing can guide physicians in selecting the safest and most effective pain management strategies.
Benefits of Personalized Medicine for Patients and Healthcare Providers
Improved Patient Outcomes By tailoring treatments to the individual patient, personalized medicine can significantly improve outcomes. Patients are more likely to receive treatments that work for them, reducing the trial-and-error approach often seen in traditional medicine.
Cost-Effectiveness Although personalized medicine involves advanced testing and data analysis, it has the potential to reduce healthcare costs in the long run. By selecting the most effective treatments from the start, patients can avoid costly complications and hospitalizations associated with ineffective therapies.
Preventive Care and Early Diagnosis Personalized medicine also emphasizes prevention, using genetic testing and biomarkers to identify individuals at high risk for certain conditions. By intervening early, doctors can prevent diseases from developing or progressing, leading to better health outcomes and reduced healthcare costs.
The post Revolutionizing Healthcare: The Rise of Personalized Medicine appeared first on .
]]>